Publications / Academic Output
My work is divided into research on research, research on and using simulation, and most recently, research on the human microbiome.

Fink R, Kuhn K, Yanez ND, Taekman JM The relationship of Grit to faculty evaluations and standardized test scores of anesthesia residents: a pilot study MedEdPublish, 7, [4], 52, 2018.
Taekman, JM, and R Bonakdar.. Integrative Pain Management Must Include Diet Considerations. Anesthesia and Analgesia, May 2018.
McGrath JL, Taekman J, Dev P, Danforth DR, Mohan D, Kman N, et al. Using Virtual Reality Simulation Environments to Assess Competence for Emergency Medicine Learners. Fernandez R, editor. Academic Emergency Medicine. 1st ed. 2017 Sep 9;48(Suppl 1):101.
Taekman J, Foureman MF, Bulamba F, Steele M, Comstock E, Kintu A, et al. A Novel Multiplayer Screen-Based Simulation Experience for African Learners Improved Confidence in Management of Postpartum Hemorrhage. Front Public Health. 2017;5:248.
Taekman JM. To Take Care of Patients Well, Physicians Must Take Care of Themselves. Academic Medicine 2017 Apr;92(4):427. PMID: 28350594
MC Wright, S Dunbar, BC Macpherson, EW Moretti, G Del Fiol, J Bolte, JN Taekman, N Segall, Toward Designing Information Display to Support Critical Care A Qualitative Contextual Evaluation and Visioning Effort, Appl Clin Inform. 2016 Oct 5;7(4):912-929. PMID: 27704138 DOI: 10.4338/ACI-2016-03-RA-0033
Deutsch ES, Dong Y, Halamek LP, Rosen MA, Taekman JM, Rice J. Leveraging Health Care Simulation Technology for Human Factors Research: Closing the Gap Between Lab and Bedside. Hum Factors. 2016 Jun 6. pii: 0018720816650781. [Epub ahead of print] PMID: 27268996
Segall N, Bonifacio AS, Barbeito A, Schroeder RA, Perfect SR, Wright MC, Emery JD, Atkins BZ, Taekman JM, Mark JB. Operating Room-to-ICU Patient Handovers: A Multidisciplinary Human-Centered Design Approach. Jt Comm J Qual Patient Saf. 2016 Sep;42(9):400-14. PMID: 27535457
Mary IH Cobb MD, Jeffrey M Taekman MD, Ali R Zomorodi MD, L Fernando Gonzalez MD, Dennis A Turner MM. Simulation in Neurosurgery – a brief review and commentary. World Neurosurgery. Elsevier Ltd; 2015 Dec 15;:1–19.
Udani AD, Moyse D, Peery CA, Taekman JM. Twitter-Augmented Journal Club: Educational Engagement and Experience So Far. A A Case Rep. 2015 Nov 17.
Segall N, Hobbs G, Granger CB, Anderson AE, Bonifacio AS, Taekman JM, et al. Patient Load Effects on Response Time to Critical Arrhythmias in Cardiac Telemetry. Crit Care Med. 2015 May;43(5):1036–42. doi: 10.1097/CCM.0000000000000923
Haga SB, Mills R, Aucoin J, Taekman JM. Interprofessional education for personalized medicine through technology-based learning. Personalized Medicine. 2015 Jun;12(3):237–43.
Wright MC, Segall N, Hobbs G, Phillips-Bute B, Maynard L, Taekman JM. Standardized Assessment for Evaluation of Team Skills: Validity and Feasibility, Simulation in Healthcare. (accepted for publication March 5, 2013). We developed a Standardized Assessment for Evaluation of Team Skills (SAFE-TeamS) in which actors portray health care team members in simulated challenging teamwork scenarios. This research sought to provide evidence of the validity and feasibility of SAFE-TeamS as a tool to support the advancement of science related to team skills training. Thirty-eight medical and nursing students were assessed using SAFE-TeamS before and after team skills training. SAFE-TeamS scores reflected improvement following training and were sensitive to individual differences. SAFE-TeamS was sensitive to individual differences and team skill training, providing evidence for validity. SAFE-TeamS provides a method to measure INDIVIDUAL team skills (rather than groups of providers).
Bonifacio AS, Segall N, Barbeito A, Taekman JM, Schroeder R, Mark JB. Handovers from the OR to the ICU. Int Anesthesiology Clinics. 2013;51(1):43–61. 22.
Segall N, Kaber DB, Taekman JM, Wright MC. A cognitive modeling approach to decision support tool design for anesthesia provider crisis management. International Journal of Human-Computer Interaction. 2013; 29(2):55-66.
Segall N, Bonifacio AS, Schroeder RA, Barbeito A, Rogers D, Thornlow DK, Emery J, Kellum S, Wright MC, Mark JB, on behalf of the Durham VA Patient Safety Center of Inquiry. Can we make postoperative patient handovers safer? A systematic review of the literature. Anesthesia and Analgesia. 2012; 115(1):102–115.
Corvetto MA, Taekman JM. To Die or Not To Die? A Review of Simulated Death. Simul Healthc 2012. There is considerable controversy over whether to allow a simulator to die during a session when death is not a predefined learning objective. In this narrative review, we survey the literature on simulated death during health care training, present arguments for and against the broad incorporation of such training in curricula for health care providers, and outline recommendations for using death scenarios in health care simulation.
Corvetto MA, Hobbs GW, Taekman JM. Fire in the Operating Room. Simul Healthc. 2011 Dec;6(6):356-9.
Frederick HJ, Corvetto MA, Hobbs GW, Taekman J. The “Simulation Roulette” Game. Simul Healthc. 2011.
Taekman JM and Stafford-Smith M, Velazquez EJ, Wright MC, Phillips-Bute BG, Pfeffer MA, Sellers MA, Pieper KS, Newman MF, Van de Werf F, Diaz R, Leimberger J., Califf RM. Departures from the protocol during conduct of a clinical trial: a pattern from the data record consistent with a learning curve. Qual Saf Health Care. Oct 2010;19(5):405-410.The VALsartan In Acute myocardial iNfarcTion, a large multinational, pragmatic, randomized, double-blind, multi-center trial, was retrospectively evaluated for evidence of research conduct consistent with a performance “learning curve.” 12 367 patients at 931 sites were analyzed. Departures (protocol violations and deviations) were more common for patients enrolled earlier at a site (p<0.0001). A similar pattern existed for queries. We concluded that research performance improved during the VALsartan In Acute myocardial iNfarcTion consistent with a “learning curve.” Although effects were not related to a change in outcome (mortality), learning curves in clinical research may have important safety, ethical, research quality and economic implications for trial conduct.
Taekman JM, Shelley K. Virtual environments in healthcare: immersion, disruption, and flow. Int Anesthesiol Clin. Summer 2010;48(3):101-121. An overview of virtual environments and serious games in healthcare. Describes current applications as well as a potential future road-map for their use in healthcare.
McQueen-Shadfar L, Taekman JM, Say What You Mean to Say: Improving Patient Handoffs in the OR and Beyond, Simulation in Healthcare, 2010 August 5(4) (printed online ahead of print, July 2, 2010), doi: 10.1097/SIH.0b013e3181e3f234
Corvetto MA, Taekman JM. Recognizing and treating malignant hyperthermia. Simul Healthc. Jun 2010;5(3):169-172.
Hobgood C, Sherwood G, Frush K, et al. Teamwork training with nursing and medical students: does the method matter? Results of an interinstitutional, interdisciplinary collaboration. Qual Saf Health Care. Apr 27 2010.doi: 10.1136/qshc.2008.031732. A randomized controlled trial of four pedagogical methods commonly used to deliver teamwork training and measured the effects of each method on the acquisition of student teamwork knowledge, skills, and attitudes.The authors recruited 203 senior nursing students and 235 fourth-year medical students (total N 438) from two major universities for a 1-day interdisciplinary teamwork training course. All participants received a didactic lecture and then were randomly assigned to one of four educational methods: didactic (control), audience response didactic, role play and human patient simulation. Student performance was assessed for teamwork attitudes, knowledge and skills .Each of the four modalities demonstrated significantly improved teamwork knowledge and attitudes, but no modality was demonstrated to be superior. No modality demonstrated a significant change in teamwork skill behavior. This was the largest study to date comparing four pedagogical methods of teamwork training, a critical component of modern healthcare curricula.
Wright MC, Phillips-Bute BG, Petrusa ER, Griffin KL, Hobbs GW, Taekman JM. Assessing teamwork in medical education and practice: relating behavioural teamwork ratings and clinical performance. Med Teach. Jan 2009;31(1):30-38. Our main objective was to test the hypothesis that observer ratings of team skill will correlate with objective measures of clinical performance. Nine teams of medical students were videotaped performing two types of teamwork tasks: (1) low fidelity classroom-based patient assessment and (2) high fidelity simulated emergent care. Team skills and clinical skills were rated. There was moderate to high correlation between observer ratings of team skill and checklist-based measures of team performance for the simulated emergent care cases. These results provide prospective evidence of a positive relationship between observer ratings of team skills and clinical team performance in a simulated dynamic health care task.
Wilson K, Salas E, Rosen M., Taekman JM, Augenstein, J, Games doctors play: Guiding principles for using simulations to train shared cognition. Cognitive Technology, 2008, 13(2), 8-16.
Sinz EH, Taekman JM. New educational technology. Int Anesthesiol Clin. Fall 2008;46(4): 137-150.
Hanson NA, Hobbs E, Taekman JM. Effective management of sarin exposure: simulation case scenario. Simul Healthc. Fall 2008;3(3):204-207.
Sposito JA, Hobbs E, Taekman J. Keep it flowing: a simulation involving defective anesthetic gas delivery equipment. Simul Healthc. Winter 2007;2(4):241-245.
Taekman JM, Hobbs E, Wright MC. Intraoperative apnea: medication error with disclosure (simulation case scenario). Simul Healthc. Spring 2007;2(1):39-42.
Wright MC, Phillips-Bute B, Mark J, Stafford-Smith M, Grichnik K, Andregg BC, Taekman JM, Time of day effects on the incidence of anesthetic adverse events. Qual Saf Health Care 2006;15(4):258-63. We hypothesized that time of day of surgery would influence the incidence of anesthetic adverse events (AEs). Clinical observations reported in a quality improvement database were categorized into different AEs that reflected (1) error, (2) harm, and (3) other AEs (error or harm could not be determined) and were analyzed for effects related to start hour of care. As expected, there were differences in the rate of AEs depending on start hour of care. Our results indicate that clinical outcomes may be different for patients anesthetized at the end of the work day compared with the beginning of the day. Although this may result from patient related factors, medical care delivery factors such as case load, fatigue, and care transitions may also be influencing the rate of anesthetic AEs for cases that start in the late afternoon.
Wright, MC, Taekman JM, and Barber L, Hobbs G, Newman MF, Stafford-Smith M, The use of high-fidelity human patient simulation as an evaluative tool in the development of clinical research protocols and procedures, Contemp Clin Trials. Dec 2005;26(6):646-59. A step-by-step description of of high-fidelity simulation applied to clinical trials. Provides a description of methods with a particular sponsor and how our work impacted the overall design of the clinical trial.
Wright MC, Taekman JM, and Endsley MR, Objective measures of situation awareness in a simulated medical environment. Quality and Safety in Healthcare, 2004. 13(suppl_1): p. i65-71. A widely cited paper that provides an overview of a safety concept from aviation applied to medicine.
Taekman JM, Hobbs GH, Barber L, Phillips-Bute B, Wright MC, Newman MF, Stafford-Smith M, Preliminary Report on the use of High-Fidelity Simulation in the Training of Study Coordinators Conducting a Clinical Research Protocol, Anesthesia and Analgesia, Vol. 99, No. 2, 2004, 521-527. We hypothesized the addition of an interactive simulation exercise to standard training methods would increase the confidence of study coordinators. Eighteen study coordinators completed pre- and post exercise confidence questionnaires.A significant increase in overall confidence was seen in the simulation group. We confirmed that addition of a simulation exercise to the training of study coordinators resulted in increased confidence in their abilities to carry out the trial. The first description of an area we are pioneering at Duke: the use of high-fidelity simulation to improve the design and implementation of clinical trials.
Taekman JM, Kingsley CP, Shelley KH, Medical Education over the Internet, Academic Medicine,Vol. 71, No. 5, May 1996, p525.

Computer Resources in Regional Anesthesia Workshop, Anatomic Foundations for Pain Medicine and Regional Anesthesia, sponsored by The American Society of Regional Anesthesia, Hershey, Pennsylvania, September 13, 1997.
Continuing Medical Education: Past, Present, and Future, Fuqua School of Business, Duke University, Durham, North Carolina, September 14, 2000.
Intellectual Property, The Internet, and Higher Education, Fuqua School of Business, Duke University, Durham, North Carolina, September 17, 2001.
Handheld Computers in Medical Practice, North Carolina Association of Nurse Anesthetists District I Educational Meeting, Sheraton Imperial Hotel, Raleigh, North Carolina, March 31, 2001.
Flying Into the Future: The Duke University Human Simulation and Patient Safety Center, Invited Lecture, Human Factors and Ergonomics Society Carolina Chapter, Raleigh, North Carolina, February 18, 2002.
Duke University Human Simulation and Patient Safety Center and the Pharmaceutical Industry, Department of Continuing Medical Education, Duke University, Duke/Industry Advisory Board, Durham, North Carolina, March 6, 2002.
Mobile Regional Anesthesiology, Invited Lecture, Mobile Technology Fair, Chapel Hill, North Carolina, March 18, 2002.
Flying Into the Future: Duke University Human Simulation and Patient Safety Center, Invited Lecture, Duke University Center for Instructional Technology Showcase, Durham, North Carolina, April 25, 2002.
Should Residents Have Internet Access in the Operating Room? Invited Lecture, Society for Education in Anesthesia Spring Workshop, Durham, North Carolina, May 31, 2002.
Simulation Script Writing, Society for Education in Anesthesia Spring Workshop, Durham, North Carolina, June 1, 2002.
Simulation and Continuing Medical Education, CME Leadership in the 21st Century, Duke University, Durham, North Carolina, September 24, 2002.
Workshop on Critical Incidents and Team Interactions, Simulation Workshop, ASA Annual Meeting, Orlando, Florida, October 14, 2002.
Workshop on Electronic Resources and Simulation Design, International Meeting of Medical Simulation, San Diego, California, January 11, 2003.
Handheld Computers in Medical Practice (invited lecture), Michigan Society of Anesthesiologists, Troy, Michigan, April 26, 2003.
Educational Technology: Merging Life-Long Learning with Clinical Practice (invited lecture), Michigan Society of Anesthesiologists, Troy, Michigan, April 26, 2003.
Can or Should Simulators be used to Assess Resident Competence for Anesthetic Practice? Panel presentation, American Society of Anesthesiologist’s Annual Meeting, San Francisco, California, October 15, 2003.
Flying Into the Future: Simulation in Medical Education (invited lecture), Innovations in Medical Education: Project Medical Education Congressional Staff Luncheon, Association of American Medical Colleges, Washington, D.C., October 20, 2003
Simulation and Continuing Medical Education, CME Leadership in the 21st Century, Duke University, Durham, North Carolina, October 28, 2003.
Educational Technology and Medical Education, Medical Alumni Weekend CME program, Duke University, Durham, North Carolina, November 1, 2003.
PDAs in Anesthesia Practice Workshop (invited workshop), Society for Ambulatory Anesthesia Annual Meeting, Seattle, Washington, April 29, 2004.
Critical Incidents Simulation Workshop (invited workshop), Society for Ambulatory Anesthesia Annual Meeting, Seattle, Washington, April 30, 2004.
Regional Simulation Workshop (invited workshop), Society for Education in Anesthesia Annual Meeting, Harrisburg, Pennsylvania, June 5, 2004.
3D Standards for Medical Education and Assessment, Panel: Use and Value of an Open 3D Standard for Medical Applications: Impact, Plans and Progress of the Medical Working Group of the web3D Consortium, Medicine Meets Virtual Reality, Long Beach, California, January 29, 2005.
Can Dummies Improve Clinical Research? (invited lecture), Acurian 2005 webinar Series, March 10, 2005. https://www.acurian.com/nws_home_page.jsp
Bringing web Based Morbidity and Mortality Grand Rounds to Life Using High-Fidelity Simulation, International Conference on Healthcare Ergonomics and Patient Safety, Florence, Italy, March 31, 2005.
Flying into the Future: Simulation in Healthcare (invited lecture), Anesthesia and Surgery Joint Grand Rounds, University of Missouri, Columbia, Missouri, April 20, 2005.
3D-i-MD: Gaming, Simulation, and Learning in Healthcare, Friday Visualization Forum, Duke University Visualization Technology Group, Durham, North Carolina, April 22, 2005.
Maximizing Human Performance in Clinical Trials: Replicating Clinical Research Protocols with High-Fidelity Simulation (invited workshop), Improving Processes for Cost and Contract Management, Cambridge, Massachusetts, May 16, 2005.
Assessment for Interactive Training Applications (invited panelist), Serious Games Summit, Washington, D.C., October 31, 2005.
Panel on Serious Games/3-D Interactive Environments (moderator), International Meeting on Medical Simulation, San Diego, California, January 15, 2006.
Workshop on Serious Games: the Oxymoron Problem, International Meeting on Medical Simulation, San Diego, California, January 16, 2006.
Serious Games: Digital Game-Based Learning in Higher Education (plenary session), 2006 Center for Instructional Technology Showcase, Duke University, Durham, North Carolina, April 28, 2006.
Simulation Workshop, Society for Ambulatory Anesthesia Annual Meeting, Washington, D.C., May 5, 2006.
Serious Games, Technology Integration Program for Nursing Education and Practice Meeting, Durham, North Carolina, August 7, 2007.
3DiTeams-Team Training in a Virtual Environment, Graylyn Technology Innovation in Medical Education Conference, Winston-Salem, North Carolina, September 10, 2007.
Simulation-Based Methods for the Vascular System: The Role of Simulation in Medical Education, Co-Chair, Computers in Cardiology Meeting 2007, Durham, North Carolina, October 2, 2007.
Workshop on The ASA Simulation Network: Information for Prospective Simulation Centers, American Society of Anesthesiologist Annual Meeting, San Francisco, California, October 14, 2007.
Workshop on 3DiTeams – Team Training in a Virtual Interactive Environment, American Society of Anesthesiologist Annual Meeting, San Francisco, California, October 16, 2007.
Workshop on Applying Human Factors Methods to Anesthesia Care, American Society of Anesthesiologist Annual Meeting, San Francisco, California, October 17, 2007.
TeamSTEPPS and Simulation, Second Annual TeamSTEPPS Consortium Meeting, Durham, NC, March 17, 2008.
3DiTeams: Healthcare Team Training in a Virtual Environment, Fourth Annual Games for Health Conference, Baltimore, MD, May 8, 2008.
3DiTeams: Healthcare Team Training in a Virtual Environment, First Annual North Carolina Advanced Learning Technology Summit, Durham, NC, May 13, 2008.
Serious Games, Technology Integration Program for Nursing Education and Practice Meeting, Durham, North Carolina, August 4, 2008.
Workshop on Applying Human Factors Methods to Anesthesia Care, American Society of Anesthesiologist Annual Meeting, Orlando, Florida, October 19, 2008.
Workshop on Practical Simulator Training with a View Towards MOCA for Society for Ambulatory Anesthesiology, American Society of Anesthesiologist Annual Meeting, Orlando, Florida, October 19, 2008.
Learning in the Age of Bits and Bytes, Stead Memorial Lecture Keynote, Medical Alumni Weekend / Department of Medicine Grand Rounds, Durham, North Carolina, October 23, 2008.
Cutting Edge 3-D Virtual Environments for the Health Care Professional, Leadership Symposium on Digital Media in Health Care, Tampa, Florida, November 22, 2008.
Immersive Learning and Human Factors Research to Improve Patient Safety (invited lecture), Duke Medicine’s Fourth Annual Patient Safety and Quality Conference, Durham, North Carolina, December 12, 2008.
Grant and Proposal Writing, Post-Graduate Course, International Meeting on Simulation in Healthcare, Orlando, Florida, January 11, 2009.
State-of-the-Art Serious Games and Virtual Environments in Healthcare, International Meeting on Simulation in Healthcare, Orlando, Florida, January 12, 2009.
Determining the Efficacy of Serious Games, International Meeting on Simulation in Healthcare, Orlando, Florida, January13, 2009.
The Role of Simulation in Clinical Trial Design and Training, GlaxoSmithKline, Research Triangle Park, North Carolina, March 23, 2009.
The Role of Simulation in Clinical Trial Design and Training, Johnson and Johnson Exploratory Meeting, Duke University, Durham, North Carolina, April 15, 2009.
3DiTeams: Healthcare Team Training in a Virtual Environment, Johnson and Johnson webcast, Duke University, Durham, North Carolina, June 17, 2009.
The Role of Simulation in Clinical Trial Design and Implementation, Simulation in Medical Education Lecture Series, Stanford University, Palo Alto, California, June 25, 2009.
Learning in the Age of Bits and Bytes, Second Annual Emerging Technologies in the Operating Room Conference, Orlando, Florida, June10, 2009.
Serious Games and Simulation in Healthcare, Second Annual Emerging Technologies in the Operating Room Conference, Orlando, Florida, June 10, 2009.
Melding Games and Simulation for Healthcare, Games for Health Conference, Boston, Massachusetts, June 11, 2009.
Simulation and Patient Safety, Foundation for Anesthesia Education and Research Lecture, American Society of Anesthesiologists Annual Meeting, New Orleans, Louisiana, October 19, 2009.
Could a Game Save Your Life? HealthCampRDU (Keynote), Blue Cross-Blue Shield Campus, Durham, North Carolina, May 14, 2010.
Human Factors and Simulation: A Collaborative Model to Advance Medical Education and Patient Safety, AAMC IQ Initiative Meeting – Integrating Quality: Linking Clinical and Educational Excellence, Chicago, Illinois, June 3, 2010.
Pro Con Debate- The Mannequin Should Die, 25th Annual Society for Education in Anesthesiology Meeting, Pittsburgh, Pennsylvania, June 6, 2010.
SIM-FIT MI: Simulation for Improved Teamwork in Myocardial Infarction: Innovative In Situ Simulation and Educational Program for Improved Myocardial Infarction Care, Teamwork and Communication Subject Matter Expert, Winston-Salem, NC, November 30, 2010.
To Die or Not To Die: That is the Question, International Meeting on Simulation in Healthcare, New Orleans, Louisiana, January 24, 2011.
Addressing the First Patient Effect: The Role of Simulation in Clinical Trial Design and Training, International Meeting on Simulation in Healthcare, New Orleans, Louisiana, January 25, 2011.
Simulation and Immersive Learning: Capabilities Presentation, Boehringer Ingleheim, Durham, NC, April 7, 2011.
Simulation and Immersive Learning: Capabilities Presentation, Genentech, webEx Teleconference, August 10, 2011.
SIM-FIT MI: Simulation for Improved Teamwork in Myocardial Infarction: Innovative In Situ Simulation and Educational Program for Improved Myocardial Infarction Care, Teamwork and Communication Subject Matter Expert, Winchester, VA, September 22-23, 2011.
Simulation and Immersive Learning: Capabilities Presentation, Bristol-Meyers Squibb, Lawrenceville, New Jersey, November 20, 2011.
Simulation Business Models (Invited Panel Member), American Association of Medical Colleges Annual Meeting, Denver, Colorado, November 8, 2011.
Education is Broken, Grand Rounds, Department of Anesthesiology, University of North Carolina, Chapel Hill, North Carolina, December 11, 2011.
In Situ Simulation and Educational Program to Improve Teamwork and Door-to-Balloon (D2B) Times in Regional STEMI Systems (Expert Panel-Hall LL, Beaudin-Seller E, Dalski C, Wright MC, Taekman JM) International Meeting on Simulation in Healthcare, San Diego, California, January 30, 2012.
Assessing Healthcare Teamwork Skills in Simulation (SimPros-Wright MC and Taekman JM), International Meeting on Simulation in Healthcare, San Diego, California, January 30, 2012.
To Die or Not To Die: That is the Question (Debate-Doerr H, Sinz E, Taekman JM), International Meeting on Simulation in Healthcare, San Diego, California, January 31, 2012.
Utilizing social networking/web 2.0 tools to better serve the needs of your learners and your research, teaching and communications (Workshop-Dong Y, Taekman JM, Bauman E), International Meeting on Simulation in Healthcare, San Diego, California, January 31, 2012.
Virtual Environments in Healthcare, Military Modeling and Simulation Consortium Meeting, Travis Air Force Base, California, February 16, 2012. Included briefing of Dr. Jonathan Woodson, Assistant Secretary of Defense for Health Affairs.
Education is Broken (Keynote Address), Teaching with Technology, Georgia Health Sciences University, Augusta, Georgia, March 22, 2012.
Use of Innovative Learning in Healthcare: What is being done today and what can be done tomorrow? Experiential Learning in Healthcare Meeting, Baylor University Medical Center, Dallas, Texas, April 13, 2012.
Social Media and Simulation, International Meeting of the Society for Simulation in Healthcare. Orlando, Florida. January 2013.
Taking Meeting Notes that Really Work, Panel on Professional and Personal Workflows, MacWorld, San Francisco, California, January 31, 2013.
Duke Human Simulation and Patient Safety Center Capabilities and Projects, Federal Medical Simulation and Training Consortium Meeting, Virtual Learning Center, February 20, 2013.
Virtual Environment Facilitator Training, Flinders University of Nursing and Midwifery, Adelaide, South Australia, April 9, 2013.
Virtual Environment Facilitator Training, Gawler Health Service Centre, Gawler, South Australia, April 10, 2013.
Virtual Environment Facilitator Training, Flinders Medical Center, Adelaide, South Australia, April 11, 2013.
Virtual Environment Facilitator Training, Flinders Medical Center, Adelaide, South Australia, April 12, 2013.
Virtual Environment Facilitator Training, Flinders Medical Center, Adelaide, South Australia, April 15, 2013.
Is Education Broken? Grand Rounds, Women’s and Children’s Hospital, Adelaide, South Australia, April 17, 2013.
Is Education Broken? TeamSTEPPS Master Trainer Faculty Workshop, Hindmarsh Education Centre, Adelaide, South Australia, April 17, 2013.
Virtual Environment Training, Flinders Medical Center, Adelaide, South Australia, April 18, 2013.
Human Simulation and Patient Safety Center Capabilities: Virtual Environments and Serious Games, American Board of Anesthesiology, Raleigh, North Carolina, June 11, 2013.
Human Simulation and Patient Safety Center Capabilities: Virtual Environments and Serious Games, American Board of Anesthesiology Board Meeting, Raleigh, North Carolina, July 19, 2013.
Simulation in Fellowship Training, Society for Academic Anesthesiology Associations, Philadelphia, Pennsylvania, November 1, 2013.
Education is Broken, University of North Carolina, Chapel Hill Simulation Seminar, Chapel Hill, North Carolina, January 14, 2014.
Screen-based simulation as a method for improving postpartum hemorrhage outcomes in a low-income country, 2015 Symposium for Scaling Innovations in Global Health, Durham, NC, March 20, 2015.
The Promise of Virtual Environments and Serious Games in Healthcare, 13th Annual Safar Symposium, University of Pittsburgh, Pittsburgh, PA, May 22, 2015.

K Ruskin, Y Iwase, J Taekman, A Proposal: An Anesthesia Internet Society, World Congress of Anesthesiology, Sydney, Australia, 1996.
Blackburn TW, Schwentker MC, Grubb MR, Taekman JM, Russell GB. Subcortical potential fails to detect ischemia at C1-C2, 7th Annual Meeting of the American Society of Neurophysiologic Monitoring, St. Louis, MO, May 1996.
Haluck RS, Taekman JM, Henry J, Marshall RL. Advanced Trauma Life Support Using Simulators and web-Based Education. Medicine Meets Virtual Reality 2000, Newport Beach, California, 2000.
Taekman JM, Temo JM, Hobbs GH. MedicalSim-L: An Internet Discussion List for Human Simulation, International Meeting on Medical Simulation, Santa Clara, California, 2002.
Taekman JM, Andregg B. SimDot: An Interdisciplinary web Portal for Human Simulation, International Meeting on Medical Simulation, San Diego, California, 2003.
Taekman JM, Temo JM, Hobbs GH. Integration of PGY-1 Anesthesia Residents in Simulation Development, International Meeting on Medical Simulation, San Diego, California, 2003.
Macleod DB, Martin G, Taekman JM, Grant SA, Breslin DS, D’Ercole FJ, Lineberger CK Assessment of CA-1 Resident Peripheral Nerve Block Experience and Performance. Regional Anesthesia and Pain Medicine. 2003. Vol 28 (2) A22.
Taekman JM, Hobbs GH, Phillips-Bute B, Newman M, Stafford-Smith M. Increased Confidence in Research Coordinators Conducting a Clinical Trial Following Simulation Training, American Society of Anesthesiologist’s Annual Meeting, San Francisco, California, October 14, 2003.
Wright MC, Taekman JM. Human patient simulators as a human factors research tool in patient safety. In: Association. IE, ed. International Ergonomics Association XVth Triennial Congress and the 7th Joint Conference of the Ergonomics Society of Korea/Japan Ergonomics Society. Seoul Korea, 2003.
Hobbs GW, Andregg BC, Adrian RJ, Taekman JM, Olufolabi AJ, Time Management and the Role of a Simulation Coordinator, International Meeting on Medical Simulation, Albuquerque, New Mexico, 2004.
Howes BL, Hobbs GW, Andregg BC, Taekman JM, Fried EB, Keifer JC, Comparison of the Pharmacokinetic Models of a Human Patient Simulator and an Independent Software Model: Implications for Scenario Scripting, International Meeting on Medical Simulation, Albuquerque, New Mexico, 2004.
Olufolabi AJ, Hobbs GW, Andregg BC, Adrian RJ, Taekman JM, Promoting Trainee Experience: From the OR to the Simulator, International Meeting on Medical Simulation, Albuquerque, New Mexico, 2004.
Wright MC, Taekman JM, Barber L, Newman MF, and Stafford-Smith M. The Role of Simulation in the Development of Clinical Research Protocols. American Society of Anesthesiologists, Las Vegas, Nevada, October 2004.
Wright MC, Andregg BC, Mark JB, Stafford-Smith M, Grichnik KP, Phillips-Bute B, Taekman JM: Effects of time of day and surgery duration on adverse events in anaesthesia. In: Tartaglia R, Bagnara S, Bellandi T, Albolino S., Eds. International Conference on Healthcare Systems Ergonomics and Patient Safety, Florence, Italy: Taylor & Francis; 2005:377-380
Taekman JM, Hobbs GW, Wright MC, and Andregg BC, Management Interface-Simulation: A web-Based Calendar and Resource Reporting System for Simulation Centers. International Meeting on Medical Simulation, Miami Beach, Florida, January 2005.
Wright MC, Stafford-Smith M, Mark JB, Phillips-Bute B, Taekman JM, Association of Surgery Duration with the Incidence of Adverse Events in Anesthesia, American Society of Anesthesiologist Annual Meeting, Atlanta, Georgia, October 2005 Anesthesiology 2005;A1274.
Wright MC, Taekman JM, Griffin KL, Hobbs GW, Petrusa ER. Assessment of Team Coordination Skills in Medical Education and Clinical Practice. American Association of Medical Colleges Research in Medical Education Conference. Seattle, WA; Nov. 1, 2006.
Wright MC, Luo X, Richardson WJ, Leonard MM, Hohenhaus MM, Taekman JM, Frush KS. Piloting team training at Duke University Health System. Proceedings of the Human Factors and Ergonomics Society 51st Annual Meeting. Santa Monica, CA: Human Factors and Ergonomics Society; 2006: 949-953.
Stolp BW, Taekman JM, Hobbs GW, Simulation, ACGME and the Hyperbaric Fellowship, Abstract of the Undersea and Hyperbaric Medical Society, Inc. Annual Scientific Meeting. Ritz-Carlton Kapalua Maui, Hawaii, June 14-16, 2007.
Hobbs GW, Taekman JM, and Stolp BW. Feasibility of Simulation Training for Hyperbaric Team Skills, Abstract of the Undersea and Hyperbaric Medical Society, Inc. Annual Scientific Meeting. Ritz-Carlton Kapalua Maui, Hawaii, June 14-16, 2007.
Segall N, Taekman JM, Mark JB, Hobbs GW, Wright MC. Coding and visualizing eye tracking data in simulated anesthesia care. In Proceedings of the Human Factors and Ergonomics Society 51st Annual Meeting. Baltimore MD. Human Factors and Ergonomics Society, October 2007: 765-769.
Segall, N, Wright MC, Taekman, JM. Human patient simulation as a research tool in cognitive engineering. In Proceedings of the IEEE International Conference on Systems, Man, and Cybernetics, Montreal, Canada, October 2007: 2256-2260.
Segall N, Swaminathan M, Taekman JM, Stafford-Smith M, Wright MC. Visual attention of anesthesia providers during low and high workload phases of care. Anesthesiology. 2007; 107: A1605.
Wright MC, Segall N, Mark JB, Hobbs G, and Taekman JM. Analyzing and Visualizing Eye Tracking Data in Simulated Anesthesia Care. Anesthesiology. 2007; 107: A1111. Wright MC, Mark JB, Segall N, Hobbs G, and Taekman JM. Situation awareness of anesthesia providers during simulated patient care. Anesthesiology. 2007: 107: A1803.
Wright MC, Mark JB, Segall N, Hobbs G, and Taekman JM. Simulation scenario design and development to support human performance research in anesthesia. Anesthesiology. 2007: 107: A1115.
Taekman JM, Segall N, Hobbs G, and Wright MC. 3DiTeams – Healthcare team training in a virtual environment. Anesthesiology. 2007: 107: A2145.
Taekman JM, Segall N, Hobbs G, and Wright MC. 3DiTeams – Healthcare team training in a virtual environment. The Journal of the Society for Simulation in Healthcare. 2008:3(5) Supplement:112.
Wright MC, Segall N, Mark JB, Hobbs G, D’Alonzo R, Ten-Clay S, Taekman JM, Simulation scenario realism and difficulty for human performance research in anesthesia. The Journal of the Society for Simulation in Healthcare. 2008:3(5) Supplement:112.
Taekman JM, Segall N, Hobbs G, and Wright MC. 3DiTeams – Healthcare team training in a virtual environment, American Association of Medical Colleges, Group on Information Resources; Professional Development Conference, May 2, 2008.
Segall N, Wright MC, Hobbs G, Taekman JM. Validity and reliability of the Skills Assessment For Evaluation of Teams (SAFE-Teams) tool. Anesthesiology. 2009; 111: A1065.
Wright MC, Segall N, Hobbs G, Taekman JM. Assessing TeamSTEPPS skills: Initial evaluation of a Skills Assessment For Evaluation of Teams (SAFE-Teams) tool. In the TeamSTEPPS National Collaborative, June 3-4. Omaha, NE: National Implementation of TeamSTEPPS, 2009.
Wright MC, Segall N, Mark JB, Taekman JM. Qualitative and task analytic methods to support comprehensible intelligent system design. Paper presented at ISDA 2009, Ninth International Conference on Intelligent Systems Design and Applications, Pisa, Italy, 2009.
Segall NS, Wright MC, Turner DA, Hobbs G, Maynard L, and Taekman JM. Virtual healthcare environments and traditional interactive team training: A comparison. Agency for Healthcare Research and Quality Annual Conference, September 27, 2010.
Segall NS, Wright MC, Turner DA, Hobbs G, Maynard L, and Taekman JM. Virtual Healthcare Environments vs. High-Fidelity Mannequin-Based Team Training: A Comparison of Skill Acquisition, International Meeting on Simulation in Healthcare, New Orleans, Louisiana, January 25, 2011.
Spinner DS, Walter JW, Vazquez-Gragg M, Bloise T, Stafford-Smith M, Faulkner EC, Taekman JM, Clinical Trial Learning Curves Affect Outcomes Measurement, Patient Safety and Trial Success: Contributing Factors and a Potential Solution in Clinical Trial Simulation, ISPOR, Baltimore, MD, May 22, 2011.
Wright MC, Dawodu M, Segall,N, Taekman JM, Mark JB, Anesthesia Crisis Alerting: A Qualitative Study Toward Understanding the Complexity of Crisis Identification, American Society of Anesthesiologist’s Annual Meeting, Chicago, Illinois, October 16, 2011.
Wright MC, Segall N, Hobbs G, Turner DA, Taekman JM, Teamwork Skill: Can a Simulation-Based Team Skill Assessment Identify Individuals who will Benefit from Training? American Society of Anesthesiologist’s Annual Meeting, Chicago, Illinois, October 18, 2011.
Taekman JM, Wright MC, Stafford-Smith M, Integrating Mannequin-Based Simulation in Clinical Research Trials: Where the Rubber Meets the Road, American Society of Anesthesiologist’s Annual Meeting, Chicago, Illinois, October 18, 2011.
Spinner, D.S., D. Mladsi, J. Walter, R. Ziemiecki, M. Stafford-Smith, Taekman JM, and E. Faulkner. Clinical Trial Learning Curves May Impact Both Clinical and Economic Outcomes and Influence Health Technology Assessment and Reimbursement Decision Making, ISPOR 14th Annual European Congress, Madrid, Spain, November 5-8, 2011.
Lockhart E, Allen T, Gunatilake R, Hobbs G, and Taekman JM. Use of Human Simulation for the Development of a Multidisciplinary Obstetric Massive Transfusion Protocol, International Meeting on Simulation in Healthcare, San Diego, California, January 31, 2012.
Taekman JM, Fink R, Wright MC, Mark J, Barbeito A, Bonifacio A, Schroeder R, Hobbs G, Bartz R, Steele M, Muir H, Turner D. A Multimodal Simulation Approach to the Centers for Medicare & Medicaid Services Regulation 482.52: Sedation and Rapid Sequence Intubation for the Non-anesthesia Provider, International Meeting on Simulation in Healthcare, San Diego, California, January 31, 2012.
McMahan R, Steele M, Fink R, Turner D, Taekman JM, Identification of Subject-Matter-Expert Effort Required for the Development and Validation of Healthcare Training-Based Virtual Environments, International Meeting for Simulation in Healthcare, Orlando, Florida, January 2013.
Wright MC, Dunbar S, Moretti EW, Schroeder RA, Taekman JM, Segall N. Eye-Tracking and Retrospective Verbal Protocol to Support Information Systems Design. Proceedings of the International Symposium of Human Factors and Ergonomics in Healthcare. 2013;2(1):30–37.
Segall N, Dunbar S, Moretti S, Schroeder R, Taekman JM, Wright MC, Contextual Inquiry to Support the Design of Electronic Health Records, American Society of Anesthesiologists Annual Meeting, San Francisco, CA, October 14, 2013.
Lockhart, E, Allen T, Steele M, Bonifacio A, Hobbs G, Taekman JM, Development of a Multi-Player Obstetric Hemorrhage Simulation Program, Transfusion 2013.
Lockhart, E, Allen T, Steele M, Bonifacio A, Hobbs G, Taekman JM, Development of a Multi-Player Obstetric Hemorrhage Simulation Program, International Meeting for Simulation in Healthcare, San Francisco, CA, January 2014.
Demaria G, Segall N, Bonifacio A, Taekman JM, 3DiTeams Handover Initiative: Improving Handovers in Critical Care Using Human-Centered Design, International Meeting for Simulation in Healthcare, San Francisco, CA January 2014.
Segall N, Hobbs G, Bonifacio A, Anderson A, Taekman JM, Granger C, Wright MC, Simulation Remote Cardiac Telemetry Monitoring, International Meeting for Simulation in Healthcare, San Francisco, CA, January 2014.
Fink RF, Kuhn CM, Taekman JM, Grit and Residency Success: A Pilot Study, American Society of Anesthesiologists Annual Meeting, New Orleans, LA, October 11, 2014.
Segall N, Dunbar S, Moretti E, Schroeder R, Taekman JM, Wright MC, Contextual Inquiry to Support the Design of Electronic Health Records, American Society of Anesthesiologists Meeting, New Orleans, LA, October 14, 2014.

Taekman JM, Kingsley CP et al, The Penn State Anesthesia Electronic Case Conference-Letter to the Editor, Anesthesiology, Vol. 83, No. 4, October 1995, pp. 887-888.
Taekman JM, Anesthesiology web Site Review, GASNet, Anesthesiology, Vol. 86, No. 2, February 1997, p. 510.
Taekman JM, Anesthesiology web Site Review, Medical World Search, Anesthesiology, Vol. 8, No. 1, January 1998, p. 288.
Taekman JM, web Alert, Current Anesthesiology Reports Nov 1999 1;1(1): p. 3.
Taekman JM, web Alert, Current Anesthesiology Reports Jan 2000 1; 2(1): pp. 3-4.
Taekman JM, web Alert, Current Anesthesiology Reports Mar 2000 1; 2(2): pp. 90-91
Taekman JM, web Alert, Current Anesthesiology Reports May 2000 1; 2(3): p. 165.
Taekman JM, web Alert, Current Anesthesiology Reports July 2000 1; 2(4): pp. 259- 260.
Taekman JM, Educational Technology 2002 [article]. ASA Newsletter, May 2002 66(5): pp. 7-8.
Taekman JM, Wright MC, Time of Death? (invited manuscript), AHRQ webMM. Available at: http://webmm.ahrq.gov/. September 2005.
Taekman JM, Let the Games Begin, Pittsburgh Post-Gazette, July 31, 2011.
Taekman JM, Learning from MTV, News and Observer, August 1, 2011.
Taekman JM, Antibiotics, Obesity and You, Huffington Post, September 17, 2015. http://goo.gl/viDSYx
Taekman JM, The dangers of antibiotic overuse disrupting delicate body balance, News and Observer, September 17, 2015. http://goo.gl/zRX4Si

Chapters in books:
Blackburn TW, Taekman JM, Cronin AJ, Russell GB, In: (Ed) Russell GB. Anesthesia Considerations for Interventional Neuroradiology, Alternative Site Anesthesia: Clinical Practice Outside the Operating Room, Stoneham, MA. Butterworth Heinemann, 1st edition, 1997; 195-224.
Cronin A, Taekman JM, Functional Brain Imaging: Anesthetic Concerns, In: (Ed) Russell GB. Alternative Site Anesthesia: Clinical Practice Outside the Operating Room, Stoneham, MA. Butterworth Heinemann, 1st edition, 1997; 101-114.
Russell GB, Taekman JM, Cronin A, Anesthesia and Magnetic Resonance Imaging. In: (Ed) Russell GB. Alternative Site Anesthesia: Clinical Practice Outside the Operating Room, Stoneham, MA. Butterworth Heinemann, 1st edition, 1997; 69-82.
Wright MC and Taekman JM (2003). Human patient simulators as a human factors research tool in patient safety. Proceedings of the XVth Triennial Congress of the International Ergonomics Association and the 7th Joint Conference of the Ergonomics Society of Korea/Japan Ergonomics Society. Seoul Korea: International Ergonomics Association.
Owens TR and Taekman JM Virtual Reality, Haptic Simulators, and Virtual Environments, In: The Comprehensive Textbook of Healthcare Simulation. Springer; 2013:233–253.
Non-refereed publications:
SimBlog and SimSingularity – Information resources for individuals interested in human simulation (http://blog.simsingularity.com/ ) 2005 – present.
WiPPPBlog (Workflows in Personal and Professional Productivity) - Academic productivity tips and tricks ( http://wippp.com/blog/ ), 2012 - present
Taekman JM, Take Meeting Notes that Really Work, Macworld Magazine, July 2013. http://goo.gl/9sfQ6l
Taekman, JM, Thoughts on Open Access and Traditional Publication, January 10, 2016. http://goo.gl/pHLeXc
Taekman, JM, Mindfulness and Medicine, March 27, 2016. http://goo.gl/rmCDPb
Taekman, JM, Thoughts on the book, “Salt, Sugar, and Fat” by Michael Moss, April 23, 2016. http://goo.gl/vNbImg

Education over the Internet, First Annual Joseph Priestley Lecture, Hershey, Pennsylvania, December 6, 1995.
Facilitator, Anesthesia and the Internet, Enhancing Your Effectiveness: A Workshop for Medical Educators, Penn State University Department of Anesthesia, Hershey, Pennsylvania, January 6, 1996.
Neurophysiologic Monitoring Equipment, Section on Physics and Monitoring, Grand Rounds, Penn State University Department of Anesthesia, Hershey, Pennsylvania, January 18, 1996.
Internet for Hospital Communicators, Key presenter, Milton S. Hershey Medical Center, Hershey, Pennsylvania, May 15, 1996.
Cerebral and Spinal Cord Basics, Section on Neuroanesthesia, Resident Educational Seminars, Penn State University College of Medicine, Hershey, Pennsylvania, February 12, 1997.
Intracranial Vascular Surgery, Section on Neuroanesthesia, Resident Educational Seminars, Penn State University College of Medicine, Hershey, Pennsylvania, March 5, 1997.
Introduction to Neural Monitoring, Resident Education Curriculum Lecture, Department of Anesthesiology, Duke University Medical Center, Durham, North Carolina, April 19, 2000.
Information Gathering, Resident Education Curriculum Lecture, Department of Anesthesiology, Duke University Medical Center, Durham, North Carolina, July 19 and 26, 2000.
Introduction to Informatics, Resident Education Curriculum Lecture, Department of Anesthesiology, Duke University Medical Center, Durham, North Carolina, October 4, 2000.
Quality of Medical Information on the Internet, Resident Education Curriculum Lecture, Department of Anesthesiology, Duke University Medical Center, Durham, North Carolina, October 11, 2000.
Introduction to Simulation Laboratory, Medical Student Introductory Lecture to Cellular Biology / Physiology Laboratory, Duke University School of Medicine, Durham North Carolina, April 11, 2001.
Discriminative Weighting: A New Form of Peer Review for Electronic Environments, Internet Advisory Committee, Duke University School of Medicine, March 14, 2001.
Introduction to the Duke University Human Patient Simulator, Executive Committee of the School of Medicine, Duke University School of Medicine, March 6, 2001.
Educational Technology @ Duke, Grand Rounds Presentation, Department of Anesthesiology, Duke University, Durham, North Carolina, January 9, 2002.
Proposed Information Technology Goals for the Duke University School of Medicine Curriculum, Division of Clinical Informatics, Duke University, Durham, North Carolina, June 19, 2002.
Handheld Computers in Medical Practice, Second Year Medical Student Lecture, Duke University, Durham, North Carolina, August 8, 2002.
Duke Human Simulation and Patient Safety Center: Flying into the Future, Grand Rounds, Duke University Department of Anesthesiology, Durham, North Carolina, November 6, 2002.
Human Performance in Clinical Trial Design and Training, Responsible Conduct of Research Forum, Duke University, Durham, North Carolina, November 2, 2005.
3DiTeams-Healthcare Team Training in a Virtual Environment, Duke Simulation Symposium, Searle Center, Duke University, Durham, North Carolina, October 23, 2008.
Simulation and Patient Safety, Department of Internal Medicine, Division of Geriatrics, Duke University, Durham, North Carolina, November 23, 2008.
Learning and Teaching Styles, Department of Anesthesiology, Division of Cardiothoracic Anesthesiology, Faculty Development Series, May 5, 2009.
The Role of Simulation in Clinical Trial Design and Training, Duke Clinical Research Institute, Durham, North Carolina, May 13, 2009.
Learning and Teaching Styles, Fellows Lecture Series, Department of Anesthesiology, July 22, 2009.
Addressing the First Patient Effect: The Role of Simulation in Clinical Trial Design and Training, Duke Clinical Research Institute, Durham, North Carolina, May 13, 2009.
Learning and Teaching Styles, Fellows Lecture Series, Department of Anesthesiology, July 14, 2011.
Addressing the First Patient Effect: The Role of Simulation in Clinical Trial Design and Training, Department of Anesthesiology Grand Rounds, Durham, North Carolina, February 2, 2011.
Duke University Human Simulation and Patient Safety Center: A Collaborative Model to Advance Healthcare Education and Patient Safety, Family and Community Medicine Education Committee Meeting, Durham, NC, December 18, 2011.
The Future Role of Simulation in Anesthesia Education / Evaluation MOCA, Fellows Lecture Series, Department of Anesthesiology, May 3, 2012.
Learning and Teaching Styles, Fellows Lecture Series, Department of Anesthesiology, July 12, 2012.
Welcome to the WiPPP: Workflows in Personal and Professional Productivity, Grand Rounds, July 25, 2012.
Simulation Facilitator Training, January 10, 2013.
Simulation Facilitator Training, February 19, 2013.
The Future Role of Simulation in Anesthesia Education / Evaluation MOCA, Fellows Lecture Series, Department of Anesthesiology, April 4, 2013.
The Science and Art of Education (Pedagogy): How to Teach to the Learner’s Style, Fellows Lecture Series, Department of Anesthesiology, July 11, 2013.
Games-Based Learning in Healthcare, Innovation Seminars, Duke Institute for Healthcare Innovation, August 19, 2013.
The Science and Art of Education (Pedagogy): How to teach in the Learner’s Style, Thinkers and Leaders Department Fellow Seminar Series, July 10, 2014.
Education, Simulation, and Innovation, Thinkers and Leaders Department Fellow Seminar Series, August 21, 2014.
Simulation Facilitator Training Course, December 9-10, 2014.
Twitter Enhanced Journal Club (discussing: Devereuax et al: Aspirin in patients undergoing non-cardiac surgery), January 18, 2015
Gaming as a Tool to Develop the Next Generation of Anesthesiologists, Thinkers and Leaders Department Fellow Seminar Series, March 12, 2015.
Anesthesiology Crisis Resource Management Simulation Course for PGY-4 Residents, April 16, 2015.
Twitter Enhanced Journal Club - discussing: Sun Z1, Honar H, Sessler DI, Dalton JE, Yang D, Panjasawatwong K, Deroee AF, Salmasi V, Saager L, Kurz A. Intraoperative core temperature patterns, transfusion requirement, and hospital duration in patients warmed with forced air. Anesthesiology. 2015 Feb;122(2):276-85. doi: 10.1097/ALN.0000000000000551.), May 14, 2015.
Simulation Facilitator Training Course, June 10-11, 2015.
Mindfulness, the Basics, Thinkers and Leaders Fellows Symposium, March 17, 2016.
Simulation Facilitator Training Course, March 22-23, 2016
Sim Projects Gallery
Over the last two decades, much of my work has focused on using technology to improve healthcare education and patient safety.

LE@D is a three-dimensional, collaborative world accessible from any Internet-connected computer that provides an innovative, interactive “front-end” to distance education in the health care professions. ILE@D maximizes face-to-face interactions between teachers and students through self-directed, team-based, and facilitator led preparatory activities in the virtual environment. While in the beginning phases of development, we have a grand vision for building a generic education framework which can support a variety of inter-professional healthcare training scenarios.
Every year, approximately 500,000 people in the United States experience an ST-elevation myocardial infarction (STEMI). Prompt reperfusion is essential to minimize morbidity and mortality. Most STEMI patients are initially brought to outlying hospitals and then, if appropriate, transferred to a hospital capable of performing angioplasty. A large percentage of STEMI-patient transfers take longer than the time recommended for optimal care. Timely transfers require precise teamwork and communication between EMS, Hospitals, and STEMI-care teams.
The Duke University Human Simulation and Patient Safety Center partnered with the American College of Cardiology (ACC) to deliver an in-situ simulation educational program throughout North Carolina focused on improving door-to-balloon time in STEMI care. The program, using in situ simulation, probed weaknesses in the STEMI-care chain and aimed to improve care by enhancing teamwork and communication.

This Virtual Experience is designed to educate and train users how to identify the signs and symptoms of a Stroke. During the course, students will perform a neurological assessment of the patient; through history and examination. A virtual Neuro Exam will be completed to gain an understanding of basic neuroanatomy and neurophysiology. They will be required to identify the functional areas impacted by neuroanatomy and recognize the location of neurological dysfunction. The student will also manage the patient, by developing a plan of care. Through this patient simulation, the users will gain valuable experience in diagnosing and treating a patient presenting stroke symptoms.

Patient transfers (handovers) from surgery to intensive care units (ICUs) are known to be fraught with communication and technical errors: barriers in care which multiple studies highlight a relationship between the quality of handovers and patient outcomes.
The Human Centered Design of Handovers/Virtual Handovers project aims to improve communication and decrease preventable adverse events related to OR to Neuro-ICU handovers. The project will achieve this through the development and use of a web-based, modular, multi-modal education platform which will include instructional videos and an interactive, immersive “virtual handover game.” As a modular platform, material can be added to address all types of handovers from shift-to-shift to more unit-specific processes.
The virtual handover game was developed using a human centered design: a methodology that incorporates feedback from users throughout the development process. This process allows users to shape the design product and enhance its usability, as well as allowing them to be closely involved in the refinement of their own handover process. As part of the HCD process, focus groups were conducted with key members in the neuro ICU and OR. Feedback from the focus groups were then analyzed via conventional content analysis and integrated into the educational program.
Feedback collected through the focus groups and analyzed via conventional content analysis will be integrated into a multimodal educational program including 3DiTeams (a virtual environment for learning and practice), on-site clinical observations and technology-mediated coaching. This educational program aims to improve handover quality and patient safety in critical care. The final product will be a modular program that can be expanded to address all types of handovers from shift-to-shift to more unit-specific processes (in this case OR to Neuro ICU).
After the launch of the education program, an educational research study will be conducted to evaluate the role of mentorship in the retention of teamwork behaviors.
The study aims to provide pilot data for the research hypothesis that mentoring will slow the decay of learned teamwork and communication behaviors to greater extent than self-study alone or no intervention.

Traditional approaches to training in education include classroom style delivery and workshops--known to be mostly ineffective. Virtual simulation is an alternative method of education to teach teamwork and communication skills and knowledge.
SimX leveraged our ILE@D Hemorrhage software and was introduced to staff and students at two health sites within South Australia Health and to Flinders University. The project was funded by Health Workforce Australia funded grant through the Simulated Learning Environments Program.

Postpartum Hemorrhage (PPH) is a 3D, multi-player, instructor-facilitated virtual simulation platform designed to train teams of clinicians in the medical management of postpartum hemorrhage as well as effective teamwork and communication behaviors.
Users may choose to participate in the exercise as physicians or nurses, the facilitator, or choose to be invisible as an observer. A user may even elect to be the voice of the patient.
PPH is set in a realistic virtual birthing suite where learners can freely move about and interact with the patient, equipment, supplies, and other items in the environment through an intuitive interface of on-screen buttons or item highlights. The game allows learners to perform medical procedures such as fundal massage as well as deliver routine and emergency medications and fluids.

An inter-professional team in the Human Simulation and Patient Safety Center (HSPSC) received a 1-year, $25,000 research award from the Social Entrepreneurship Accelerator at Duke (SEAD) for a project entitled “Postpartum Hemorrhage Education Via Simulation”.
The team is pioneering the use of scalable, distributable healthcare simulation using commercial game technology with a multi-player module that specifically addresses postpartum hemorrhage (PPH). As a proof-of-concept for global health, the PPH simulation software will be used to address gaps in care at Mulago International Referral Hospital in Kampala, Uganda, and to decrease disparities in healthcare education. We will host inter-professional, interactive, games-based simulation training sessions from Durham to Mulago using the Internet. This pilot program aims to reduce the incidence of postpartum hemorrhage, and to serve as a broader model for using simulation to scale education and to spread virtual learning through the developing world in resource-poor settings. Additionally, we hope to use preliminary data to support a future proposal to study the efficacy of screen-based/games-based learning in global health. Key personnel include: Jeff Taekman (MD) who is the Principal Investigator, Megan Foureman (CRNA, MSN), Amy Mauritz (MD), Adeyemi Olufolabi (MB.BS; DCH; FRCA), Michael Steele (BS) and Genevieve DeMaria (BS).

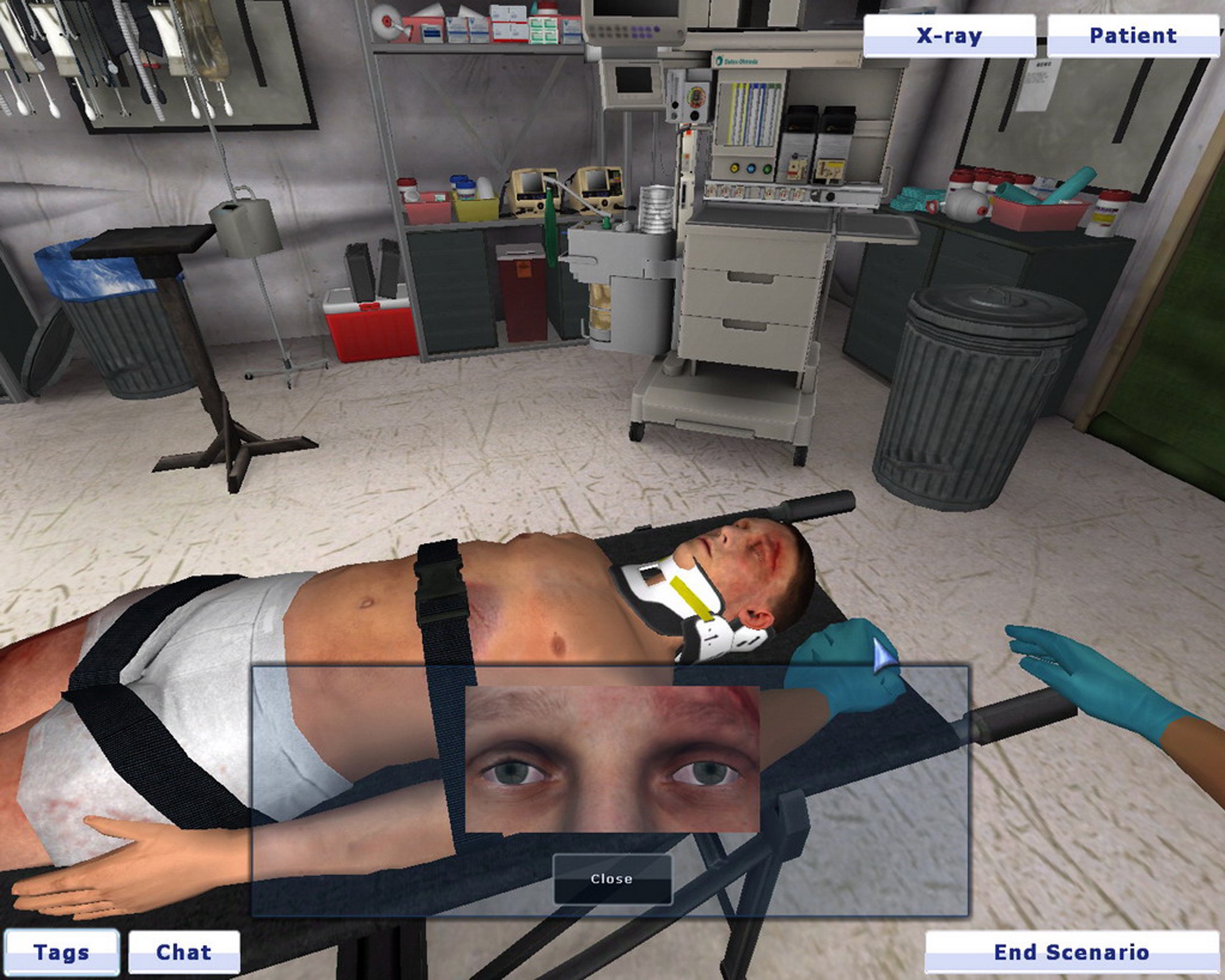
Combat Medic is an exciting new virtual educational program designed to train Army medics and other military medical personnel to manage the top causes of death in the modern battlefield: hemorrhage, airway obstruction, and tension pneumothorax (2014). Designed as a procedural trainer, the game allows medics to cognitively apply, practice, and review Tactical Combat Care, patient management, and documentation in a contextually accurate combat scenario. Combat Medic also allows for the application of other important concepts such as equipment preparation, team organization, and communication through unique and intuitive user interfaces that preserve both contextual, cognitive, and task fidelity.
Learners can either practice independently as a single player or use its multi-player function for facilitator-led and team events. Opportunities to learn reflectively is made possible with virtual pre- and post-game meeting spaces and a robust debriefing platform replete with analysis of task performance and video playback. To maximize deployability and access, the game works from browser plug-ins that are compatible with any recently produced computer.

The Pre-Deployment Anesthesia and Anaphylaxis Training System (PDAATS) -- also known as ILE@D Sedation-is a serious game designed to teach and refresh the cognitive skills of rapid sequence intubation and moderate / deep sedation to non-anesthesia providers.
This single-player, first-person simulation enables clinicians to evaluate, sedate, and medically manage ten different patients each with a unique set of medical and contextual challenges. In each scenario, learners must identify and interpret relevant findings in the patient’s background and physical exam to determine primary and secondary sedation plans.
Each patient avatar is innervated by the HumanSim physiology engine which accurately and dynamically generates heart rate, respiratory rate, blood pressure, and blood oxygen saturation depending on the learner’s actions. Cognitive fidelity is further enhanced through an innovative interface that allows learners to select medications, medication dosages, and delivery.
Following the simulation, a robust after action review (AAR) that allows players to reflectively learn from their performance.
Effective team coordination is critical for the safe delivery of care. Development of these skills requires training and practice in an interactive team-based environment. A three-dimensional serious game environment provides an engaging and cost effective alternative to other interactive training solutions such as human patient simulation. In this project we are developing a three-dimensional interactive networked system for training of military health care team coordination skills. Although this is a development project with no formal experimental hypothesis, we will conduct qualitative evaluations of the design specification and alpha and beta versions of a demonstration prototype. Ease of use, practicality, scope, and effectiveness of the training system will be assessed through heuristic analysis by experts in team training.
Tech Projects Gallery

A TwitterJC provides a platform for residents and the global anesthesiology community to engage in education, share expertise, and generate an enduring resource for the anesthesia community.

Prior to the finalization of a complex protocol and/or during the start up of a study that has unique training needs, we will institute the use of the Duke Human Simulation and Patient Safety Center (HSPSC) for two distinct purposes; protocol “usability”/design, and immersive training of research personnel.
Researchers in the HSPSC have demonstrated phenomenon consistent with learning curves in the data record of several clinical trials1 and have described the benefits of applying simulation techniques in the development and start-up of clinical trials.2,3 There is emerging evidence that learning curves may negatively influence the outcome of large multicenter clinical trials4 and the frequency of adverse events.5 The HSPSC is pioneering the use of human factors methods and simulation to mitigate learning curves in clinical trials. The application of our methods provide long term benefits to patients, trainees, and sponsors, including protection of the sponsors investment in their drug or device, the reduction of research cost and most importantly, reducing the potential risks to real patients. Simulation (mannequin-based or actor-based) is typically used in two ways: 1) protocol walk-throughs and 2) research personnel training.
Walkthroughs are used to assess protocol design. Protocol developers observe their study performed by research personnel in a high-fidelity simulated clinical setting prior to subject enrollment. Viewing (and reviewing) walkthroughs of clinical protocols helps uncover issues with design, timing, complexity, and practicality. Potential protocol errors and inefficiencies are highlighted and can be corrected before the protocol is implemented, thereby minimizing subject exposure and the number of protocol amendments—ultimately impacting both safety and cost.
In addition, skill acquisition of the research personnel is a key factor in the safe and effective deployment of a clinical research protocol. Proper performance of a clinical trial depends on complex behaviors. Complex human behaviors demonstrate ‘learning curves’, where performance improves with repetition. Just like a sports team, proficiency is gained through practical experience. Interactive training in a simulated environment provides the opportunity for Investigators, coordinators, and monitors to ‘practice’ without placing subjects or data at risk. Following simulation training, research personnel are closer to optimal performance at the time subject enrollment begins.
Ultimately, we believe our methods improve the chances of a successful trial (through better design and enhanced research personnel performance) while minimizing cost, improving efficiency, and enhancing safety.
Two examples of protocols using the simulation training are:
A Phase II multicenter, randomized, double-blind, parallel group, dose-ranging, effect-controlled study to determine the pharmacokinetics and pharmacodynamics of Sodium Nitroprusside in pediatric patients, sponsored by the NIH.
A Phase III, multicenter, randomized study of the safety and efficacy of Heparinase I versus Protamine in patients undergoing CABG with and without cardiopulmonary bypass/ sponsor by sponsored by an industry pharmaceutical company.
References
1. Taekman JM, Stafford-Smith M, Velazquez EJ, Wright MC, Phillips-Bute BG, Pfeffer MA, et al. Departures from the protocol during conduct of a clinical trial: A pattern from the data record consistent with a learning curve. Qual Saf Health Care 2010, Aug 10.
2. Wright MC, Taekman JM, Barber L, Hobbs G, Newman MF, Stafford-Smith M. The use of high-fidelity human patient simulation as an evaluative tool in the development of clinical research protocols and procedures. Contemp Clin Trials. 2005;26:646-659.
3. Taekman JM, Hobbs G, Barber L, et al. Preliminary Report on the Use of High-Fidelity Simulation in the Training of Study Coordinators Conducting a Clinical Research Protocol. Anesth Analg. 2004;99:521-527.

The Anesthesia Cash Register - authored this award-winning program that calculates the cost of an anesthetic in real and compressed time. Received a Meritorious Award in Stuart Pharmaceutical’s Cost-Effectiveness Awards. 1992–1993.
The Penn State Anesthesia Content Outline and Keyword Review - designed and implemented this interactive teaching tool which reviews and tests essential topics in anesthesia. Part of the 1994 ASA Annual Meeting’s First Place Scientific Exhibit. 1994–1995.
Penn State Anesthesia Home Page - designed, programmed and maintained the Penn State / Geisinger Anesthesia World Wide web Home Page and internet serving computer. 1995–1999.
Penn State Anesthesia Electronic Case Conference - peer-reviewed educational publication on the internet dedicated to the discussion of perioperative management issues in anesthesia. Chosen as charter program for Penn State’s World Campus, a global distance education initiative. 1995–1999.
Penn State Anesthesia Recruitment Kiosk - designed and programmed this computer kiosk authored to convey information on the Penn State Anesthesia Residency Program. 1995–1996.
Applied Research Ethics National Association Home Page – designed, implemented, and maintained home page for this national organization (www.aamc.org/research/primr/arena/)1995.
Anesthesia Employment Archive - designed, programmed, and maintain the original internet resource enabling position matching in anesthesia (www.anes.hmc.psu.edu/employmentfolder/AEAhome.html). 1996–1999.
Pennsylvania Society of Anesthesiologist’s Home Page - designed and programmed the Society’s World Wide web Page. 1996.
The Ontology Mine - invented this computer-based medical education and reference tool. PSU Software Disclosure No. SW-97 031. 1997–1999.
The Penn State Anesthesia Intranet – programmed, designed, and maintained this internal departmental resource. Includes database/web integration for tracking clinical time, educational time, and resident evaluations. 1997–1999.
Penn State College of Medicine Faculty Discussion Site - designed and maintained this institution-wide internet resource to disseminate and discuss issues of importance to the clinical and research faculty. 1998–1999.
ResEval - A web-Based Resident Evaluation System. 1999–2004.
Academic Relative Value Unit Project (AcademicRVU)-A web-based system to monitor faculty productivity and resources. 1999–2001.
The Comparison Matrix (CompMatrix)-A web-based decision making tool to help resident applicants compare and rank disparate anesthesiology residency programs. Software disclosure: Patent Pending. 2000–2007.
MedicalSim-L Human Simulation Discussion List– founded an international internet discussion group focusing on human simulation. Ultimately folded into the Society for Simulation in Healthcare. 2001–2006.
Simulation Scripting Template – a method for “story-boarding” simulation exercises prior to formal simulator programming. 2001–present.
Medical Student Surgical Core Palm Project – A Palm/web based tool to aid in point-of-care education for medical students and residents. 2001–2002.
Duke Anesthesiology Didactics Course Site - A web-based didactic archiving project. 2001–2003.
Faculty Profiling System/web - A web-based tool which automates the classification and identification of research interests of the Duke University School of Medicine Faculty. 2001–2002.
SimDot – A multidisciplinary, peer-reviewed, web-based community to facilitate collaboration in simulation patient and scenario development., 2002–2006.
Simulation Management Interface – designed and implemented this system used to manage the Duke University Human Simulation and Patient Safety Center. (http://dukesimcenter.org/calendar/) 2002–2008.
ACGME-Compliant PDA Case Log – designed the application framework and oversaw the development of this handheld application used to track resident cases and procedures. 2003–2004.
Peripheral Nerve Block PDA Log Book – designed the application shell and served as advisor for development of this handheld application to track regional anesthesia procedures. 2003–2004.
Medical Student Procedure PDA Log Book – designed the application shell and serve as advisor for development of this handheld application to track medical student patient and procedure encounters. 2003–2005.
News

How to be Healthier, Happier and More Productive: It's All in the Timing
by Daniel H. Pink, Wall Street Journal, December 29, 2017
Resources to stay current in your field
Commentary - Duke Clinical Practice Today - December 2015
Op-ED in Huffington Post - September 17, 2015
The dangers of antibiotic overuse disrupting delicate body balance
Op-Ed in News and Observer - September 17, 2015
Video Gaming -- A Youth Movement We Need to Get Behind
Commentary - Huffington Post - December 17, 2013
Teamwork and Communication (TeamSTEPPS) in a virtual world
Feature Promo - SimX: Government of South Australia - May 7, 2013
How to take meeting notes that really work
Article - MacWorld Magazine - Apr 16, 2013
Computer simulations allow doctors to learn skills with less risk
Medical students at Duke University are using a new virtual game-based tool to learn from their mistakes without a life depending on it. With the latest in life-like patient simulation labs, healthcare students and professionals can get hands-on experience in making life-saving decisions.
Feature Story -WRAL- March 29, 2013
VIDEO GAMES ARE TOMORROW'S ANSWER TO EXECUTIVE TRAINING
Commentary - Fast Company - March 14, 2012
How MTV has rewired the way we learn
Op-Ed - Dallas News - January 2011
How video games can make you smarter
Commentary - CNN - January 31, 2011
Commentary - Wired Magazine - August 10, 2004
Funding

Active:
5R01-HS023387-02 (P.I Segall) Effect of monitoring system design on response time to cardiac arrhythmias
Completed:
NIH 1R01-NS049548-01, National Institute of Neurologic Disorders and Stroke/Agency for Healthcare Research and Quality/Office of Research Integrity, “Defining the Learning Curve in Clinical Trials,” Principal Investigator, Funding: $267,415, 12% effort. 2004 – 2009.
Anesthesia Patient Safety Foundation,”Effect of Time of Day and Surgery Duration on Adverse Events in Anesthesia,” Co-Principal Investigator, Funding: $41,598, 2004 – 2005.
Medical Education Research Fund of the National Board of Medical Examiners, “Assessment and Prediction of Teamwork” (PI Melanie Wright), Co-Investigator, Funding: $69,718, 1% effort, 2004 – 2005.
Telemedicine and Advanced Technology Research Center (TATRC) / Office of the Secretary of Defense, “Regional Anesthesiology Trainer,” Phase I Small Business Innovation Research Grant (PI Randy Haluck, M.D., Verefi Technologies, Inc.), Consultant. Funding $99,000. 2006.
Health Resources and Services Administration, “Duke University Nurse Anesthesia Program,” (Principal Investigator Barb Turner), Simulation Director, Funding $551,007, 5% effort 2006-2009.
The Duke Endowment, Open Access Medical Education Curriculum, (Principal Investigator: Ed Halperin), Investigator, Funding $1,000,000, 1% effort, 2005 – 2007.
Anesthesia Patient Safety Foundation Research Award, “Objective Measures of Performance in Simulated Anesthesia: A Comparison of Experts and Novices,” (PI Melanie Wright), Co-Principal Investigator, Funding $79,959, 8.5% effort, 2006 – 2007.
Telemedicine and Advanced Technology Research Center (TATRC) / Office of the Secretary of Defense, “ 3DiTeams: Gaming Environment for Training Healthcare Team Coordination Skills,” Principal Investigator, Funding $249,530, 15% effort, 2006-2007.
GlaxoSmithKlein, “Collaboration Between Duke University Medical Center and the Terry Sanford Institute of Public Policy and the University of North Carolina at Chapel Hill School of Medicine and School of Public Health, Quality of Care and Patient Safety,” (Principal Investigator Karen Frush), Co-investigator, Funding $1.65 million ($225,000 for “Development of Multidisciplinary Team Training”), 10% effort, January 1, 2006 – December 31, 2008.
NIH 5U18HS016653-01, Agency for Healthcare Research and Quality, “Virtual Health Care Environments versus Traditional Interactive Team Training,” Principal Investigator, Funding $291,248, 22% effort, September 30, 2006-September 29, 2009.
Veterans Affairs Health Administration National Center for Patient Safety, Solicitation for Patient Safety Centers of Inquiry, “Improving Patient Safety during Moderate Sedation Procedures through Point of Care Simulation Training (PoCST) of Physician-Nurse Teams” (PI Jonathan Mark, MD). Co-Investigator. Total grant $575,124, 15% effort, October 2007-September 2009.
Edward J. Stemmler Medical Education Research Fund of the National Board of Medical Examiners, “Standardized Teamwork Skills Assessment: Feasibility, Reliability, and Validity,” Principal Investigator, Funding: $149,297, Effort 10%. August 2008-July 2010.
Veterans Affairs Health Administration National Center for Patient Safety, Solicitation for Patient Safety Centers of Inquiry, “Designing a Safer OR to ICU Patient Handover, ” (Principal Investigator: Jonathan Mark, MD). Co-Investigator. Total grant $575,124, 7.5% effort, October 1, 2009-September 30, 2011.
D09 HP14984, Department of Health and Human Services, “Pediatric Acute and Chronic Nurse Practitioner”, (Principal Investigator: Barbara Turner, Ph.D.), Investigator, Funding $675,569, Effort 10%, July 1, 2009-June 30, 2013. Focused on teamwork and communication behavior training through virtual environments.
Telemedicine Advanced Technology Research Center, “Virtual Anesthesiology Rapid Sequence Induction Trainer,” Funding $1.8 million, effort 10%, February 2011-June 2013. Virtual environment for training non-anesthesia provider reservists the critical skills critical in sedation and rapid sequence intubation.
R18 HS020415-01, Agency for Healthcare Research and Quality, “Creating Simulation-Based Performance Assessment Tools for Practicing Physicians” (Principal Investigator: Matthew Weinger, Vanderbilt), Funding: $1,047,706, 4/1/11 -1/30/13. Assessment in maintenance of certification programs in anesthesiology.
Government of South Australia, SimX-Virtual Learning Environment, (Duke Principal Investigator), Adelaide, South Australia, $120,000, October 2012-June 2013.
W15P7T-12-WP-VPTVW00, RDECOM, Merging Virtual Patient with Virtual Worlds Technology, Duke Principal Investigator, Funding: $152,052, October 2012-September 2014.
The Duke Endowment, “ILE@D (Immersive Learning Environment at Duke)”, (Principal Investigator: Edward Buckley, M.D.), Co-Investigator, Programmatic Lead, Funding $2.8 million, Effort 20%, 2009-2014. Focused on developing a virtual environment platform for medical and nursing school learning.
Duke Graduate Medical Education Innovation Fund, “Facilitator Training for Human Simulation,” Principal Investigator, Funding $50,460. Focused on training future facilitators in simulation.
Pfizer, Abbott, “3DiTeams Initiative—Handover training”. Principal Investigator, $750,000, December 2011-December 2015.
Anesthesia Patient Safety Foundation - Forgetting to remember: a study of prospective memory errors in the Operating Room (Principal Investigator: Noa Segall, Ph.D.)
Social Entrepreneurship Accelerator at Duke (SEAD), Postpartum Hemorrhage Education via Simulation, Principal Investigator, Funding: $25,000, November 2014-November 2015.
Clasado Biosciences Association of prebiotic consumption and perioperative anxiety
1UH4-ES027072-01 (P.I. Sempowski) Duke Infectious Disease Response Training Consortium (DIDRT)
Durham Casualty-Simulation-Based Crisis Resource Management as a Risk Reduction Strategy for the Duke Health System
Mentorship and Collaboration

My historical domains of interest–healthcare education, technology and quality are not the prototypical bench science pursuits. Those with traditional academic careers (e.g. bench scientists) have a hard time understanding what it is I do. In fact, it has been difficult to find traditional academic mentors due to the uniqueness of my niche.
Time has reinforced the true importance of mentorship. I am forever thankful to the mentors I had thus far in my career-several took an interest in me even though they didn't fully understand my passion. It has been challenging given my interest in cutting / bleeding edge technologies to find mentors at the faculty level—there simply aren’t others that do what I do. Despite this, I have had a modicum of success despite this shortcoming by seeking strong mentors that although they do not understand my domain, do excel excel at mentoring.
It is my hope, by assembling an outstanding, passionate and productive team, we will help change the definition of a 'traditional' academic career.
More importantly, I’ve tried to pass the mentoring I've received forward—and have found I especially enjoy mentoring certain types of individuals—those that have intrinsic motivation andpassion for success—qualities Angela Duckworth (another positive psychology researcher) refers to as “Grit.” Gritty individuals, in my experience, are much more likely to find success in their academic endeavors. One of my mentees, Ryan Fink, is investigating the correlation of Grit with academic success.
I’ve found an ever-expanding number of residents, nurses, fellows and young faculty are interested in developing simulation and patient safety as the focus of their academic pursuits. I receive supreme satisfaction in helping talented individuals realize their potential. I plan to expand my circle of interprofessional mentees in the next phase of my career, supporting and mentoring them .

I have many individuals to thank for their guidance and mentorship:

Noa Segall, Ph.D. (NCSU, Industrial Engineering, Faculty 2006)
Natasha Kyte (FAER Scholar, 2008)
Peter Thurlow, M.D. (Medical Student)
David Turner, M.D. (Faculty, Department of Pediatrics, 2008)
Marcia Corvetto, M.D. (Visiting Faculty, 2009-2010)
Ryan Fink, M.D. (Resident, Fellow, Faculty 2010)
Ryan McMahon, Ph.D. (post-doc, 2011-2012)
Daryl Wilcox, M.D. (Resident)
Neechi Mosha (Medical Student 2012-2013)
John Lemm, M.D. (Fellow, Faculty 2012-present )
Megan Foureman, CRNA (2013-2015)
Ankeet Udani, M.D. (Faculty, 2014-present)
Michael Fierro, M.D. (Fellow, 2015)

Noa Segall, Ph.D.
Melanie C. Wright, Ph.D.
Mark Stafford-Smith, M.D.
Joseph Mathew, M.D., MHSc, MBA
Regis Kopper, Ph.D.
Ryan Fink, M.D.
Brad Taicher, D.O., MBA
Yemi Olufolabi, M.B., B.S.
Andrea Fuimefreddo, MS
Michael Steele
Megan Foureman, CRNA
Ankeet Udani, M.D., MSEd.
Bronwyn Southwell, M.D.
Len White, Ph.D.
Constance Johnson, Ph.D.
Mark Feinglos, M.D.
John Lemm, M.D.
Mike Fierro, M.D.
Chad Grotegut, M.D., MBA, MHSc
Jennifer Justice, RN
Awards / Recognition

Meritorious Award, Stuart Pharmaceutical’s Cost-Effectiveness Award. 1993.
American Society of Anesthesiologist’s Scholar - Foundation for Anesthesia Education and Research Burroughs-Wellcome ASA Scholarship Program. 1993.
Chief Resident, Department of Anesthesia, Penn State University College of Medicine. 1994 – 1995.
First Place, Scientific Exhibits, Implementation of Cognitive Science in Anesthesiology Education and Training, American Society of Anesthesiologist’s Annual Meeting, San Francisco, California. 1994.
Continuing and Distance Education Award, Penn State University. 1995.
Arrow International Multi-Media Education in Medical Sciences Fellowship. 1997.
Editor, Anesthesiology Section, The Medical Matrix. 1999 – 2001.
Director, Informatics Education, Department of Anesthesiology. 1999 – 2005.
Editor, web Alerts, Current Anesthesiology Reports. 1999 – 2000.
Section Editor, Anesthesiaweb. 2001.
Director, Human Simulation and Patient Safety Center, Duke University School of Medicine, Durham, NC, 2001 – present.
Assistant Dean for Educational Technology, Duke University School of Medicine, Durham, North Carolina, 2001 – present.
Medical Student Teaching Award, Department of Anesthesiology, Duke University Medical Center, Durham, North Carolina, 2001.
Research Award for SimDot, 2003 Annual International Meeting on Medical Simulation, San Diego, California, 2003.
Inaugural Secretary, Society for Simulation in Healthcare. 2004 – 2006.
web Editor, Society for Simulation in Healthcare, 2004-2007.
Listserv Moderator, Society for Simulation in Healthcare, 2004-2010.
Editorial Board, Simulation in Healthcare: The Journal of the Society for Medical Simulation. 2005 - 2013.
Evaluation Board, Faculty of 1000, Technology and Monitoring Section of the Anesthesiology and Pain Management Faculty, 2007 - present.
Association of University Anesthesiologists, 2008 - present.
Planning Committee, Leadership Symposium on Digital Media in Health Care 2008, Tampa, Florida 2008.
Best Doctors 2007-2016, Elected by my peers for inclusion in the Best Doctors in America®.
Marquis Who’s Who in America, 2009, 2010, 2011.
Chancellor’s Clinical Leadership in Academic Medicine Program, 2010.
Simmy Award - Most Innovative Educational Strategy, International Meeting on Simulation in Healthcare, New Orleans, Louisiana, January 24, 2011.
Briefed the Assistant Secretary of Defense for Health Affairs (Dr. Jonathan Woodson) at the Federal Medical Simulation and Training Consortium Meeting. Travis Air Force Base, California. February 2012.
Google Glass Explorer - one of 8000 initial recipients of Google Glass to investigating applications in learning, patient care, and healthcare quality / safety.
Teaching Recognition Award - Innovation in Education - International Anesthesiology Research Society - Awarded March 2013, received May 2013 (recognizes and funds novel concepts or applications that improve educational programs and advance the practice of anesthesiology).
Lead Judge: 5th Annual Serious Games and Virtual Environment Arcade and Showcase, International Meeting on Simulation in Healthcare, New Orleans, LA, January 12, 2015.
Lead Judge: Serious Games / Virtual Environments Arcade and Showcase, Institute of Medicine’s Envisioning the Future of Health Professional Education Public Workshop of the the Global Forum on Innovation in Health Professional Education. Washington, D.C., April 23, 2015. (video...)



